PEMF Therapy for Stress Regulation

PEMF therapy for stress regulation is increasingly discussed as part of a broader nervous system wellness strategy. Rather than framing stress as something to “eliminate,” modern physiology views it as a natural response that becomes problematic when it remains chronically activated. Pulsed electromagnetic field (PEMF) therapy is being explored for its potential influence on cellular signaling, microcirculation, and autonomic balance — all of which play a role in how the body processes stress.
This guide takes a conservative, evidence-aligned look at how PEMF may interact with the stress response, what current research suggests, and where realistic expectations should be set.
Understanding the Stress Response

Stress is primarily governed by the autonomic nervous system (ANS), which regulates heart rate, breathing, blood flow, and hormonal signaling. The sympathetic branch mobilizes energy (“fight or flight”), while the parasympathetic branch promotes recovery (“rest and digest”).
According to the National Institutes of Health (NIH), chronic activation of stress pathways can influence inflammation, sleep patterns, cardiovascular tone, and mood regulation. The goal is not to suppress stress entirely, but to improve adaptability — the ability to shift efficiently between activation and recovery states.
A practical way to think about stress regulation is as a “range” rather than a single state. In day-to-day life, most people cycle through activation (work demands, family logistics, commuting) and recovery (meals, rest, sleep). When recovery periods are consistently shortened or disrupted, the body may stay biased toward sympathetic activation — showing up as shallow breathing, muscle tension, difficulty winding down, or a “wired but tired” feeling.
From a physiology standpoint, the stress response involves multiple layers:
- Fast signaling (seconds to minutes): autonomic shifts that change breathing rate, heart rate, and blood flow distribution.
- Hormonal signaling (minutes to hours): stress hormones that influence alertness, glucose availability, and immune messaging.
- Behavioral feedback (hours to days): sleep disruption, changes in appetite, reduced movement, and changes in coping habits.
Because these layers interact, “stress regulation” in a wellness context usually means supporting recovery capacity and improving the ability to return to baseline after activation — not forcing the body into calm at all times.
How PEMF Interacts with Cellular Signaling
PEMF therapy delivers low-frequency electromagnetic pulses designed to interact with cellular membranes. Research published on PubMed explores how electromagnetic fields may influence ion exchange, calcium signaling, and membrane potential stability.
These mechanisms are relevant because cellular communication underlies broader physiological processes — including nervous system tone and stress reactivity. While PEMF is not a direct “anti-stress” intervention, its interaction with cellular signaling may contribute to improved systemic regulation.
In a conservative framing, PEMF is best understood as a stimulus that may influence “how cells communicate,” rather than an intervention that dictates an outcome. Cells rely on electrochemical gradients (especially across membranes) to coordinate transport, signaling, and metabolic activity. Even small changes in ion movement can alter how tissues behave at a systems level — particularly in muscle, vascular tissue, and nerve-related signaling.
Two concepts often discussed in PEMF education are:
- Membrane potential support: a stable electrical environment across cell membranes is associated with normal cellular function and signaling efficiency.
- Signal timing: the body’s signaling systems depend on “when” messages arrive, not only “what” the message is. Pulsed exposures are studied partly because timing and rhythm may matter for biological responses.
Importantly, the scientific literature varies by device parameters (frequency, waveform, intensity, and session duration). That variability is one reason it’s more accurate to talk about plausible mechanisms and reasonable use patterns rather than promising uniform effects.
Nervous System Regulation and Autonomic Balance
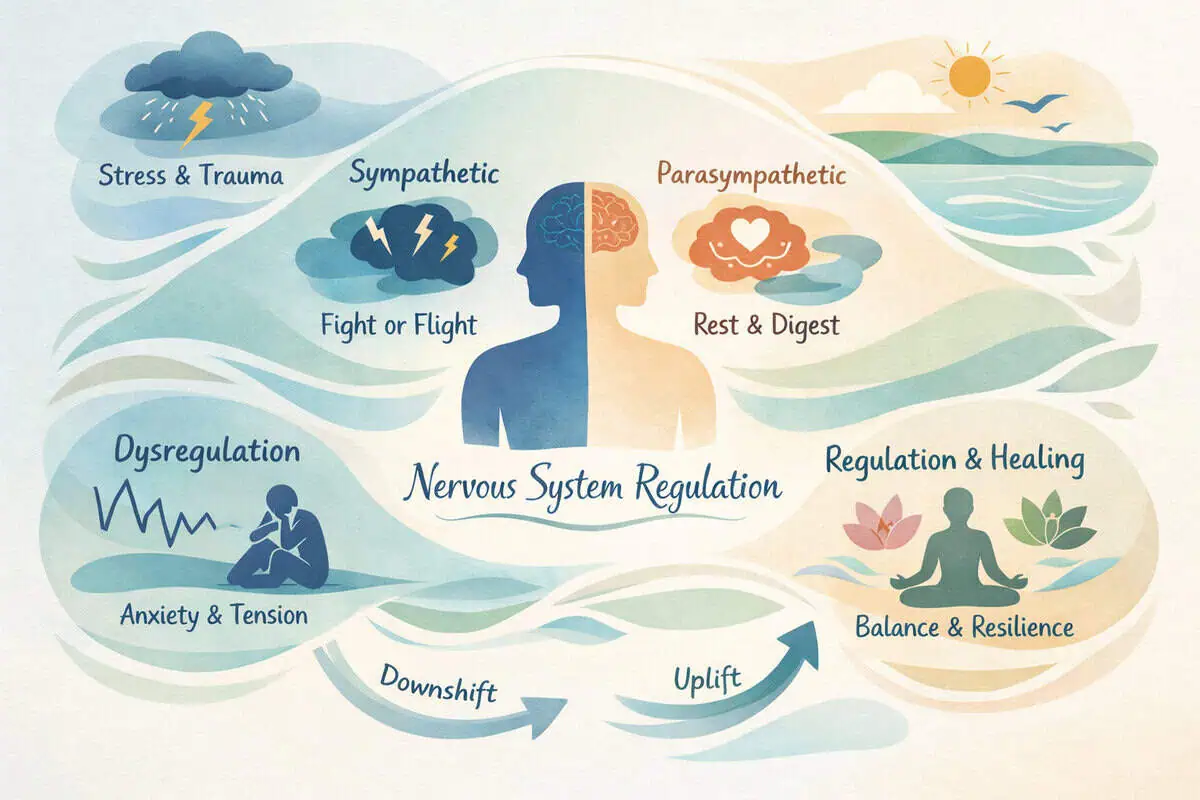
Some research suggests that electromagnetic field exposure may influence autonomic nervous system metrics such as heart rate variability (HRV), a marker often associated with stress resilience. HRV reflects the dynamic interplay between sympathetic and parasympathetic branches.
Improved autonomic flexibility does not equate to treatment of anxiety or medical conditions. Instead, it may reflect enhanced regulatory capacity — the ability of the nervous system to shift toward recovery more efficiently after stress activation.
In wellness terms, “autonomic balance” is often less about being calm all day and more about having a smoother transition into recovery when the demand drops. For example, after a stressful meeting or a long drive, a regulated nervous system tends to downshift more effectively — breathing becomes slower, muscle tone eases, and attention becomes less vigilant.
PEMF is sometimes paired with practices that directly engage parasympathetic pathways, such as slow exhalation breathing, progressive muscle relaxation, or a quiet environment. This pairing is not required, but it reflects a common logic: if PEMF is being used as a supportive tool, it may fit best when the rest of the routine is also oriented toward recovery.
From a selection perspective, many at-home users start with gentler settings specifically because strong stimulation can feel energizing rather than calming for some people. A conservative approach is to treat early sessions as “tolerance and response mapping,” paying attention to sleep timing, perceived relaxation, and how the body feels the following day.
Microcirculation and Oxygen Delivery

Microcirculation — the flow of blood through small vessels — plays a role in nutrient delivery and waste removal. Some studies have evaluated PEMF’s influence on microvascular function, which may indirectly support recovery processes associated with stress physiology.
The Cleveland Clinic notes that chronic stress can affect vascular tone and circulation. While PEMF is not a vascular treatment, its investigation in microcirculatory research suggests a possible supportive mechanism worth understanding.
Why might circulation matter for stress regulation? When stress is persistent, people may experience patterns like shallow breathing, reduced movement, and sustained muscle tension. These patterns can influence local blood flow and perceived comfort. In that context, interventions that support general recovery routines (movement, hydration, sleep, relaxation practices) may also influence perceived well-being.
A conservative way to interpret microcirculation research is as “tissue support,” not an acute calming effect. If microcirculatory function is supported over time, the body may be better positioned for recovery processes that contribute to resilience — especially when PEMF is part of a broader lifestyle strategy.
Mitochondrial Support and Energy Regulation

Stress demands energy. Mitochondria — often referred to as the “power plants” of the cell — are central to ATP production. Laboratory studies have examined how electromagnetic fields may influence mitochondrial membrane potential and oxidative balance.
Energy regulation is closely tied to resilience. When cellular energy production is efficient, the body may transition more smoothly between activation and recovery phases. This represents a potential indirect pathway through which PEMF therapy for stress regulation is being explored.
In everyday terms, energy regulation relates to how stable someone feels across the day — not “more energy” as a promise, but steadier capacity to handle demands without crashing. Stress can disrupt this through sleep fragmentation, inconsistent meals, reduced activity, and sustained vigilance. If PEMF is used as part of a consistent routine, some users view it as a way to support recovery inputs that indirectly influence energy stability (rest, relaxation, and comfort).
It’s also worth noting that responses can be individualized. Some people report feeling more alert after a session, especially if the setting is more stimulating. Others prefer using PEMF later in the day as part of a wind-down routine. This variability is one reason “start low and track response” is generally a conservative best practice.
What Users Typically Report

Users often describe:
- A subtle pulsing sensation
- A feeling of warmth or gentle relaxation
- Improved wind-down routines in the evening
- A sense of calm following consistent sessions
These observations are experiential, not medical claims. Effects vary widely, and consistency appears to be more important than intensity.
In practice, “what it feels like” can depend on device type and placement. Full-body mats may feel more immersive simply because the contact area is larger, while localized applicators (not the focus of this post) can feel more targeted. Some people notice little during a session but report that the routine itself — lying down, unplugging from screens, breathing slowly — becomes a reliable cue for downshifting.
A conservative way to interpret user feedback is to separate:
- Session effects (what is felt in the moment): pulsing, warmth, relaxation, or sometimes alertness.
- Routine effects (what changes around the session): consistency, improved evening habits, fewer late-night stimulants, or better wind-down structure.
Because stress regulation is heavily influenced by habits, many people evaluate PEMF by whether it supports a sustainable recovery routine they can repeat, rather than by chasing a dramatic immediate sensation.
Realistic Expectations and Limits

PEMF therapy should not be positioned as a cure for anxiety disorders, depression, or stress-related medical conditions. The Mayo Clinic emphasizes that stress management typically involves lifestyle factors such as sleep, exercise, social support, and cognitive strategies.
PEMF may be viewed as one supportive component within a broader wellness framework. It does not replace therapy, medication, or clinical evaluation.
Session Structure for Stress Support

Typical at-home use patterns often include:
- 10–30 minute sessions
- Low to moderate intensity settings
- Pairing sessions with breathing exercises
- Evening routines to support relaxation
For broader device comparisons and educational context, see the Best PEMF Devices & Mats (2026 Buyer’s Guide).
Long-term considerations can matter as much as the first few sessions, especially for people using PEMF as a routine support tool:
- Consistency: many wellness routines show clearer “felt” value when used regularly (for example, several sessions per week) rather than sporadically.
- Timing: evening use may fit relaxation goals, while morning or midday use may feel more energizing for some people depending on settings.
- Placement and comfort: comfort influences adherence. A mat that is easy to set up and comfortable to lie on may be used more consistently than a system that requires frequent adjustments.
- Noise, heat, and environment: even small friction points (fan noise, room temperature, clutter) can reduce follow-through, which matters for stress-focused routines.
From a practical “ownership reality” perspective, it helps to plan for:
- Maintenance: basic cleaning, storage, and safe handling of cables/connectors to avoid wear over time.
- Space and portability: whether the device stays in one location or needs to be moved frequently.
- Compliance and contraindications: re-checking safety guidance if health status changes (new implanted devices, pregnancy considerations, or other medical updates).
A conservative approach is to track a few simple markers for 2–4 weeks: whether it supports your wind-down routine, whether sleep timing becomes more consistent, and whether you feel more capable of downshifting after stressful periods. If none of these shift, it may not be a meaningful addition to your routine.
Safety Considerations

PEMF devices are generally marketed as non-invasive wellness tools. However, individuals with implanted electronic devices, pacemakers, pregnancy considerations, or complex medical conditions should consult a qualified healthcare professional before use.
For a full overview, review the PEMF Therapy Benefits (Science-Backed Overview) and related safety materials.
Safety is also about session decision-making. A conservative user profile typically starts with shorter sessions and lower settings, then adjusts gradually. If a session feels overstimulating (for example, restlessness or difficulty winding down), many users simply reduce intensity, shorten duration, or move the session earlier in the day. The goal is comfort and routine compatibility, not pushing intensity.
Integrating PEMF into a Broader Stress Strategy

Sustainable stress regulation typically includes:
- Sleep hygiene
- Physical activity
- Mindfulness or breathing practices
- Healthy social connection
- Professional support when needed
PEMF may serve as a complementary modality within this framework, not a standalone solution.
Ongoing Research and Future Directions

Research into electromagnetic field applications continues to evolve. Many studies focus on inflammation, pain modulation, and tissue recovery, while stress-specific pathways are still being explored.
For additional educational resources, visit our Blog or contact us via the Contact PEMF Sage page.
Conclusion: A Measured View of PEMF and Stress
PEMF therapy for stress regulation is best understood as a supportive wellness tool grounded in cellular and nervous system research. While emerging evidence suggests possible influences on autonomic balance, microcirculation, and energy regulation, it is not a medical treatment for stress-related disorders.
If you’re exploring device options or want a broader comparison, review our Buyer’s Guide to understand how different systems are positioned within the PEMF landscape.
