PEMF Therapy and the Nervous System

PEMF therapy and the nervous system is a topic that draws attention from individuals interested in stress regulation, relaxation, and overall physiological balance. Pulsed electromagnetic field (PEMF) devices deliver low-frequency electromagnetic signals that interact with tissues at a cellular level, potentially influencing ion exchange, microcirculation, and signaling pathways.
This guide takes a conservative, evidence-aligned look at how PEMF therapy may relate to nervous system function. We will focus on physiology, realistic expectations, and safety — not cure claims or medical treatment promises. For broader foundational context, see our overview of PEMF therapy benefits.
Understanding the Nervous System: Central and Autonomic Branches
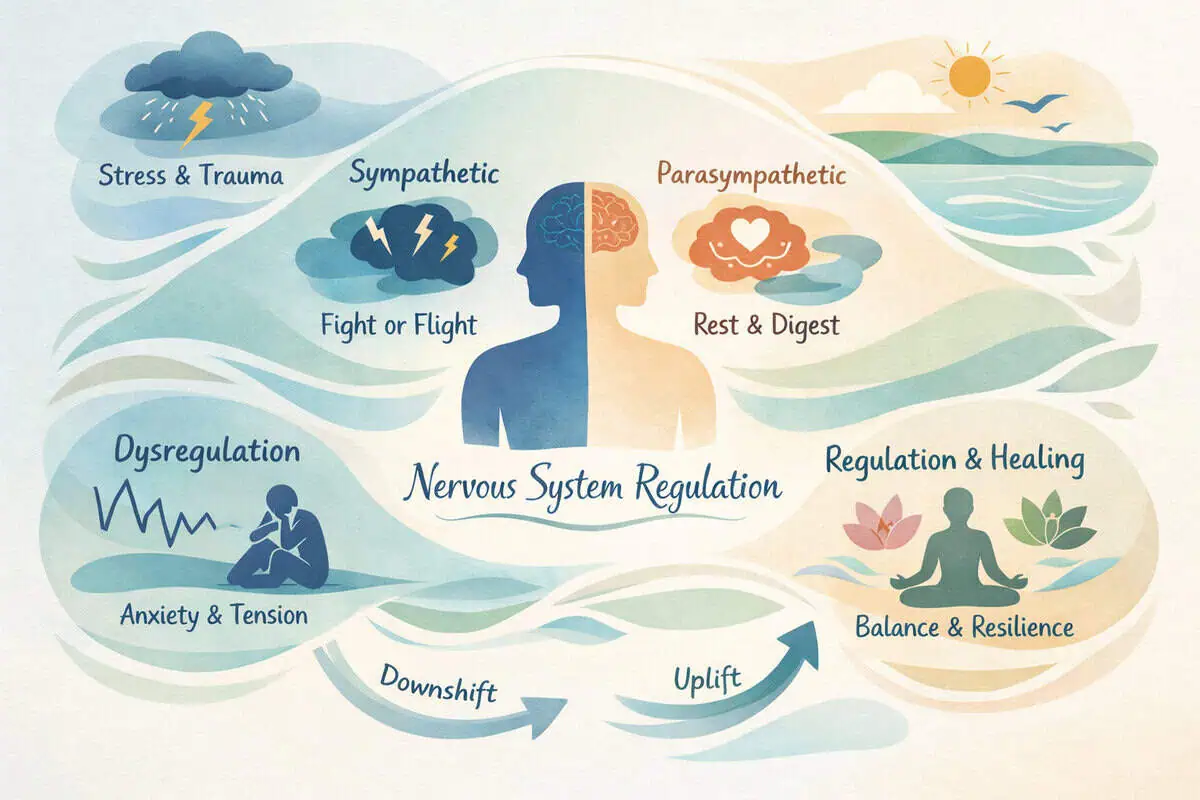
The nervous system consists of the central nervous system (brain and spinal cord) and the peripheral nervous system. A key component of interest in wellness discussions is the autonomic nervous system (ANS), which regulates heart rate, digestion, respiration, and stress responses.
The ANS includes two primary branches:
- Sympathetic: Often described as “fight or flight.”
- Parasympathetic: Often described as “rest and digest.”
Balance between these branches supports overall resilience. Dysregulation can manifest as persistent stress responses or difficulty relaxing. According to the Cleveland Clinic, autonomic imbalance may influence cardiovascular, digestive, and metabolic patterns.
From a practical perspective, it can help to think of the autonomic nervous system as an always-on “background regulator.” It continuously adjusts:
- Heart rhythm and vascular tone (how blood vessels constrict or relax)
- Breathing pattern (rate and depth, especially under stress)
- Digestive motility (how smoothly the gut moves)
- Alertness and recovery signals (when the body shifts toward rest)
This is one reason the phrase “autonomic balance” comes up in wellness conversations. It does not imply a perfect 50/50 split. Instead, it refers to flexible switching — being able to meet demands (sympathetic activation) and then downshift effectively (parasympathetic recovery).
A related concept often discussed is vagal activity (the vagus nerve is a major parasympathetic pathway). In conservative terms, “supporting vagal tone” generally means supporting the body’s ability to return to a calmer baseline after stress. This is commonly measured indirectly through markers like heart rate variability (HRV), which can reflect how responsive the autonomic system is to changing conditions.
Cellular Signaling and Electrophysiology
Nervous system communication depends on electrical gradients across cell membranes. Ion channels regulate sodium, potassium, calcium, and other ions — maintaining membrane potential and enabling signal transmission.
PEMF devices generate low-frequency electromagnetic pulses that may interact with these ion channels. Research indexed in PubMed explores how electromagnetic fields may influence cellular signaling pathways, though mechanisms remain under investigation.
It is important to distinguish between cellular-level modulation and clinical outcomes. Evidence suggests potential influence on signaling behavior, but this does not equate to disease treatment.
A useful way to frame this is to separate signal generation from signal interpretation. Neurons and support cells (like glial cells) operate within tightly controlled electrical and chemical environments. Small shifts in ion movement can influence:
- Membrane excitability (how easily a cell can “fire”)
- Calcium signaling (important for neurotransmitter release and intracellular messaging)
- Cell-to-cell communication (how networks coordinate activity)
In conservative PEMF discussions, the focus is typically on whether pulsed electromagnetic fields could provide a gentle “nudge” to these processes — not a forced override. That distinction matters, because nervous system health is less about turning one switch on and more about supporting stable, adaptable regulation.
It can also help to remember that “nervous system function” is not only about the brain. Peripheral nerves, autonomic ganglia, and local tissue environments all contribute. For example, local tissue stress, circulation changes, and inflammatory signaling can all influence how nerves behave — which is one reason PEMF discussions sometimes overlap with recovery and relaxation routines.
PEMF Therapy and Autonomic Regulation

One area of interest is how PEMF therapy may relate to autonomic balance. Some observational research suggests low-frequency electromagnetic stimulation may influence heart rate variability (HRV), a marker often associated with autonomic flexibility.
The National Institutes of Health (NIH) notes that HRV reflects interplay between sympathetic and parasympathetic activity. While PEMF is not a replacement for medical care, subtle shifts in relaxation responses are commonly reported in wellness contexts.
Typical user experiences may include:
- Gentle pulsing sensations
- A sense of calm during sessions
- Improved relaxation routines when used consistently
When HRV is discussed, it is best treated as a contextual marker rather than a “score to chase.” HRV can be affected by sleep, hydration, caffeine, alcohol, illness, training load, stress, and even measurement timing. If someone tracks HRV, the most conservative approach is to look for stable trends over weeks — not day-to-day fluctuations.
From a routine standpoint, people often explore PEMF sessions during windows when the body is already “allowed” to downshift, such as:
- After work, before dinner, or as a transition out of a stressful day
- Before a wind-down routine (low light, reduced screens, calmer breathing)
- After light movement (walking, gentle mobility) when the body is warm and relaxed
This matters because autonomic regulation is strongly influenced by context. A calm environment, comfortable temperature, and quiet breathing pattern may increase the likelihood that a session feels relaxing — regardless of device type.
Microcirculation and Neural Tissue Support

Nervous tissue relies heavily on adequate oxygen and nutrient delivery. Microcirculation — the flow of blood through small vessels — supports neuronal health.
Some research has examined whether electromagnetic stimulation may influence local circulation. Enhanced microcirculatory dynamics could theoretically support tissue recovery environments, though conclusions remain cautious and context-dependent.
For a broader commercial overview of available device categories, you may review our Best PEMF Devices & Mats (2026 Buyer’s Guide).
A conservative way to connect circulation to nervous system comfort is to remember that nerves exist within tissues that also need adequate perfusion. When microcirculation is less efficient (for many possible reasons), tissues may feel “tighter,” less resilient, or slower to recover from daily load. This does not mean PEMF “fixes” circulation. It means circulation is one plausible pathway researchers investigate when evaluating how electromagnetic stimulation could influence tissue environments.
Microcirculation also relates to autonomic signaling because vascular tone is heavily regulated by autonomic inputs. In simple terms: the nervous system helps decide when blood vessels constrict or relax. This is another reason “stress state” and “recovery state” can feel different in the body.
Mitochondrial Function and Neural Energy Demand

Neurons are metabolically active cells requiring substantial ATP production. Mitochondria are central to this energy generation.
Laboratory research has explored how electromagnetic fields may interact with mitochondrial pathways. While mechanisms are still being clarified, some models propose influence on oxidative metabolism and redox balance.
These cellular-level discussions are exploratory and should not be interpreted as medical claims. They provide theoretical context for why PEMF therapy and the nervous system are studied together.
In practical, non-medical terms, “mitochondrial support” is often discussed as supporting the body’s ability to meet energy demands and recover from stressors. For the nervous system, energy demand shows up in many places:
- Maintaining membrane potential (cells spend energy to keep ion gradients stable)
- Neurotransmitter cycling (chemical messengers are released, cleared, and recycled)
- Stress adaptation (the body shifts between alertness and recovery states)
Because PEMF research sometimes examines cellular energy and signaling together, it is reasonable to describe mitochondria as part of the “why” behind ongoing interest — while still keeping expectations measured and evidence-aligned.
PEMF Therapy in Relaxation and Daily Stress Routines

Many individuals incorporate PEMF sessions into structured relaxation routines. Sessions often last 10–30 minutes and may be paired with breathing exercises or quiet rest.
This aligns with broader behavioral strategies recommended by the Mayo Clinic for stress management, including consistent routines and parasympathetic activation techniques.
PEMF therapy may serve as an adjunct to these practices rather than a standalone solution.
If someone is experimenting with PEMF therapy and the nervous system from a wellness perspective, consistency and simplicity usually outperform complicated protocols. Conservative routine ideas include:
- Choose a predictable time (e.g., early evening) for 2–4 weeks to observe patterns.
- Keep the environment calm (lower light, reduced noise, comfortable temperature).
- Pair the session with one stable habit (slow breathing, gentle stretching, or quiet reading).
A “successful” relaxation routine does not require strong sensations. Many users report the experience as subtle, especially early on. If a session feels overstimulating, some people reduce session duration, adjust timing (earlier in the day), or focus on calmer breathing during use — always within manufacturer guidance and any medical constraints.
For people who already track sleep and recovery habits, it can help to keep a simple log (sleep timing, caffeine intake, stress level, session timing). This does not prove causality, but it supports better personal decision-making and prevents overattributing changes to a single variable.
What PEMF Therapy Is Not

PEMF therapy is not:
- A cure for neurological disorders
- A replacement for psychiatric or neurological care
- A substitute for prescribed medications
It should not be marketed or interpreted as treating anxiety disorders, depression, neurodegenerative disease, or other medical conditions. Always consult a qualified healthcare provider for diagnosis or treatment decisions.
Safety Considerations

General safety considerations include:
- Avoiding use with implanted electronic medical devices unless medically cleared
- Consulting professionals during pregnancy
- Discontinuing use if unusual discomfort occurs
For a full review of contraindications, see our PEMF Therapy Safety, Risks & Contraindications page.
Long-term, trust-first use is less about “pushing intensity” and more about ownership reality: the user is responsible for safe setup, appropriate expectations, and consistency. Conservative best practices often include:
- Follow device instructions exactly (session duration, placement guidance, and warnings).
- Keep sessions predictable before experimenting with frequency changes.
- Avoid stacking too many variables (new supplements, big training changes, and PEMF changes all at once can make outcomes hard to interpret).
Maintenance and practical considerations can matter as much as the session itself. Examples include checking cables and connectors for wear, keeping the device clean per manufacturer guidance, and ensuring the mat or applicator is used on a stable surface. None of these steps create “better results,” but they reduce the chance of avoidable issues that can disrupt consistent use.
For the nervous system specifically, it can be helpful to watch for signs of poor fit — not danger signals, but “this routine doesn’t suit me” signals — such as feeling unusually wired after late-night sessions, difficulty winding down, or increased restlessness. In those cases, a conservative approach is to shorten sessions, move them earlier in the day, and consult a clinician if there is any uncertainty, especially for individuals with complex medical histories.
What the Research Currently Suggests

Research into PEMF therapy and the nervous system spans laboratory studies, small clinical trials, and observational reports. Outcomes vary by frequency, waveform, intensity, and population.
The evidence base is evolving. Some studies suggest modulation of inflammatory signaling or autonomic markers, while others emphasize the need for larger randomized trials.
This reinforces the importance of measured expectations and evidence-aligned communication.
Who May Consider Exploring PEMF Therapy

Individuals interested in structured relaxation routines, recovery environments, or wellness experimentation may explore PEMF therapy as part of a broader strategy that includes sleep hygiene, movement, and stress management.
It may be most appropriate for those seeking complementary wellness tools — not those expecting rapid neurological change.
Setting Realistic Expectations

Realistic expectations include:
- Gradual, subtle changes
- Benefits tied to consistent use
- Results that vary by individual
PEMF therapy and the nervous system intersect primarily at the level of cellular signaling and autonomic regulation — not dramatic transformation.
You can explore additional educational articles in our Blog.
A conservative “decision framework” can also reduce frustration:
- Define the goal clearly (e.g., “support a calmer evening routine,” not “solve a medical condition”).
- Choose one measurable habit (bedtime consistency, evening screen reduction, daily walk).
- Use PEMF as a support tool within that habit for several weeks before drawing conclusions.
This approach keeps expectations aligned with how most wellness interventions work: modest, gradual changes that compound when paired with stable fundamentals.
Conclusion: A Measured View of PEMF and Neural Balance
PEMF therapy and the nervous system is an area of growing interest rooted in electrophysiology and cellular signaling research. While early findings suggest potential interactions with autonomic regulation, mitochondrial activity, and microcirculation, the evidence supports cautious interpretation.
For those considering PEMF therapy as part of a structured wellness routine, focus on conservative expectations, safety awareness, and integration with broader lifestyle strategies. For device comparisons and technical distinctions, review our Buyer’s Guide.
If you have medical complexity, implanted devices, or medication considerations, a brief clinician check-in can help ensure your approach stays appropriate and low-risk.
