PEMF Therapy for Pain Relief: Mechanisms & Limits

PEMF therapy for pain relief is frequently discussed in wellness and recovery circles. But what does the science actually support? And where are the limits?
Pulsed electromagnetic field (PEMF) therapy delivers low-frequency electromagnetic signals to the body. These signals are believed to influence cellular communication, circulation, and nervous system signaling — all of which can play a role in how pain is perceived and regulated.
In this guide, we’ll examine the plausible biological mechanisms behind PEMF therapy for pain relief, what research suggests, and what it does not claim to do. This discussion is conservative, physiology-aligned, and free of exaggerated outcomes.
Understanding Pain: More Than a Single Signal

Pain is not a single event. It is a multi-layered experience involving:
- Nociceptor activation (peripheral pain receptors)
- Inflammatory signaling
- Microcirculatory changes
- Spinal cord processing
- Brain-based perception and interpretation
According to the National Institutes of Health (NIH), pain perception involves both sensory and emotional processing. That means addressing pain often requires influencing multiple biological systems — not simply “blocking” a signal.
This systems-level view is important when evaluating PEMF therapy for pain relief. The question becomes: can electromagnetic signaling influence any of these physiological layers in a meaningful but realistic way?
One helpful way to frame pain is to separate signal generation from signal interpretation. Nociceptors can detect mechanical strain, temperature shifts, or chemical changes in tissue. But whether that input becomes “pain” depends on how the spinal cord and brain process and prioritize the information in context.
That context can include sleep quality, stress load, training volume, and prior injury history. None of this implies pain is “in your head.” It simply reflects that pain is a protective output created by the nervous system when it perceives threat or overload.
This is one reason PEMF therapy for pain relief is often discussed as supportive rather than definitive. If PEMF meaningfully influences circulation, signaling balance, or nervous system reactivity, it may shift the overall environment in which pain is processed — even if it does not directly “erase” nociceptive input.
It’s also important to recognize that pain can become sensitized over time. In some cases, the nervous system becomes more responsive to normal inputs (often described as “amplification”). This can make outcomes from any single modality variable, since the driver may be mechanical, inflammatory, neurochemical, or a combination.
Cellular Signaling & Ion Exchange
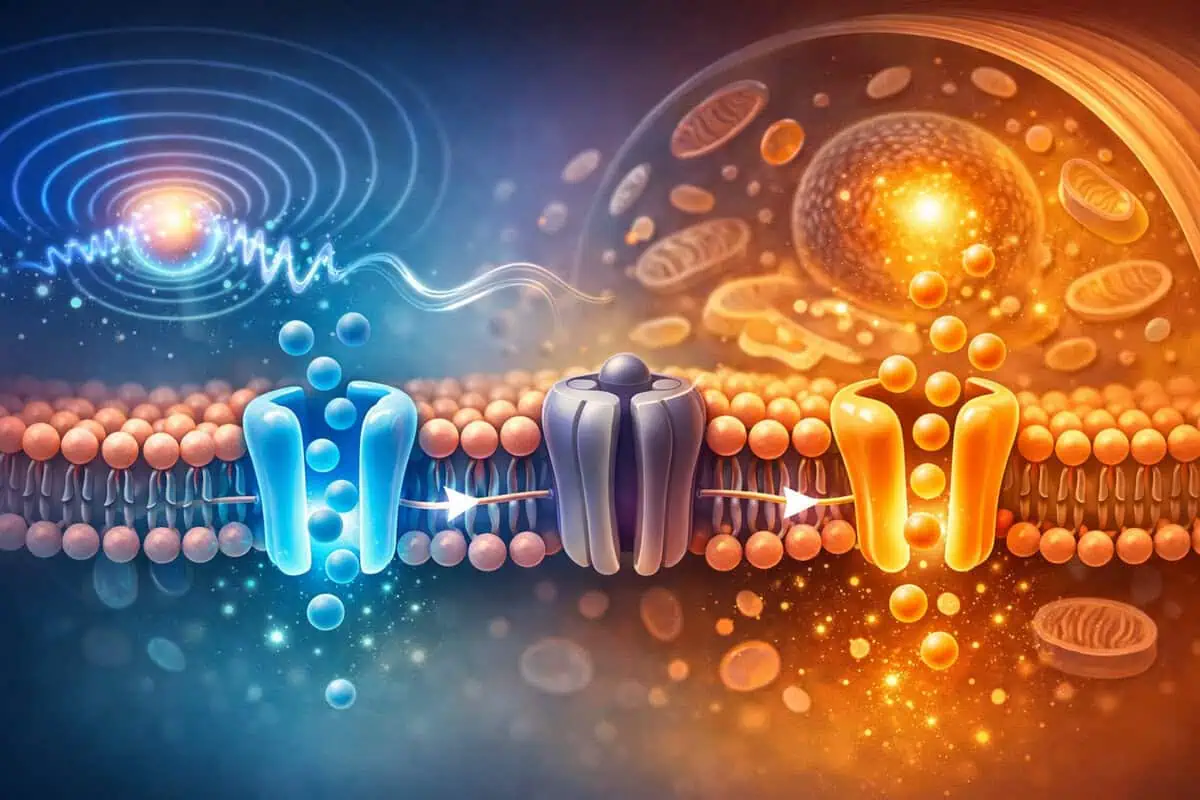
One proposed mechanism behind PEMF therapy for pain relief involves ion channel modulation. Cells rely on the controlled movement of ions (such as calcium and sodium) across membranes to regulate signaling and function.
Research indexed in PubMed suggests electromagnetic fields may influence calcium ion binding and membrane potential in certain contexts. Calcium plays a critical role in inflammatory signaling and nerve transmission.
While this does not mean PEMF “turns off pain,” it suggests a possible pathway through which electromagnetic pulses could influence cellular communication involved in discomfort signaling.
To understand why ion movement matters, it helps to remember that many cellular “decisions” are electrical at the membrane level. Nerve cells, muscle cells, and immune cells all depend on gradients of sodium, potassium, chloride, and calcium to create electrical potentials that enable communication.
In conservative terms, the theory is that external electromagnetic pulsing may nudge how some cells respond to signaling demands — for example, by influencing gating behavior of ion channels or altering the local electrochemical environment near the membrane. Even small shifts can matter because ion channels act like switches that trigger downstream signaling.
This is also why PEMF parameters vary so much across devices and studies. Frequency, waveform shape, intensity, and exposure time can change the biological interaction profile. Two protocols both labeled “PEMF” may be functionally different in the body.
A practical takeaway: when evaluating PEMF therapy for pain relief, it is more reasonable to expect subtle regulation effects that accumulate with consistent use than immediate, dramatic results from a single session.
Microcirculation & Tissue Environment

Microcirculation refers to blood flow through the smallest vessels — capillaries, arterioles, and venules. Impaired microcirculation can contribute to tissue stress and discomfort.
Some studies suggest PEMF exposure may influence vascular tone and nitric oxide pathways, which play roles in circulation. The Cleveland Clinic explains that healthy circulation supports oxygen delivery and metabolic waste removal — both relevant to tissue comfort.
Improved microenvironment conditions may help explain why some users report subtle reductions in localized discomfort during consistent use. However, outcomes vary, and PEMF should not be viewed as a replacement for medical evaluation when pain is persistent or unexplained.
Microcirculation matters because tissues are constantly balancing supply and demand. Muscles, tendons, and joints have different blood flow characteristics, and certain connective tissues are naturally slower to perfuse than highly vascular tissue. When circulation is constrained, tissues may become more sensitive to load or recovery demands.
A conservative interpretation is that PEMF therapy for pain relief may support tissue environment quality by promoting a more favorable balance of oxygen delivery, nutrient transport, and metabolic byproduct clearance. This does not imply a guaranteed effect, but it helps explain why some people associate PEMF with “feeling looser” or “less tight” after consistent use.
It is also worth noting that circulation is not only about arteries and veins. Capillary exchange and local tissue fluid dynamics influence how quickly tissues return to baseline after strain. PEMF is sometimes discussed in relation to these dynamics, but the best-supported framing remains modest: supporting normal circulation-related processes rather than claiming a direct therapeutic outcome.
Inflammation & Signaling Modulation

Inflammation is a complex signaling cascade involving cytokines, immune cells, and vascular responses. It is not inherently negative — it is part of repair and adaptation.
Some laboratory and clinical research suggests PEMF exposure may influence inflammatory markers in certain contexts. The Mayo Clinic notes that inflammation-related discomfort often stems from signaling imbalance rather than a single cause.
The conservative interpretation: PEMF therapy for pain relief may support normal inflammatory signaling regulation — not suppress it outright. This distinction matters. The goal is balance, not elimination.
In practical terms, “inflammation-related discomfort” can reflect several overlapping processes: local tissue irritation, immune signaling, changes in vascular permeability, and nerve sensitization in the surrounding area. Not all discomfort is inflammatory, but inflammation can contribute to how intense or persistent a sensation feels.
Because the inflammatory response is necessary for repair, approaches that aim to “shut it down” are not always appropriate. A more realistic goal is supporting recovery conditions so the body can progress through the normal repair cycle efficiently.
This is where PEMF is often positioned: as a low-burden input that may support signaling balance and tissue environment stability. The most conservative expectation is that this could contribute to comfort over time — especially when paired with basics like sleep, appropriate movement, and load management.
Nervous System Regulation
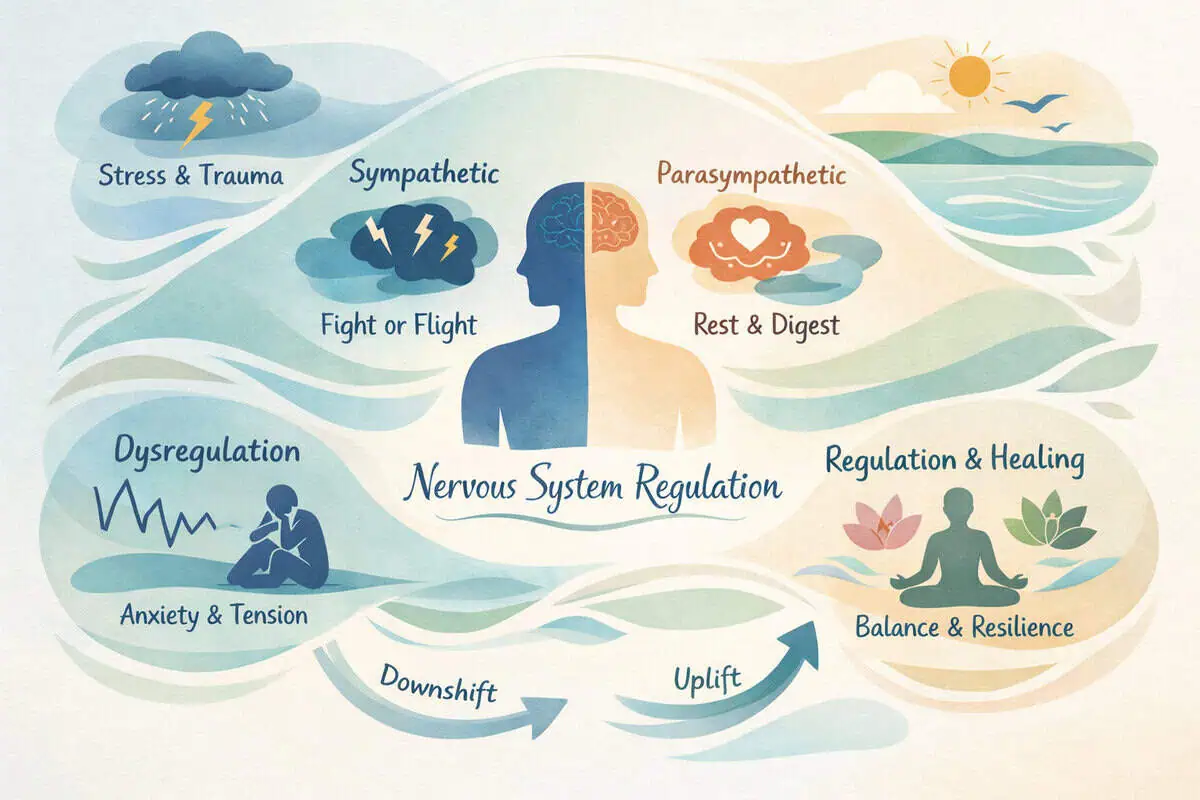
Pain perception is deeply connected to the autonomic nervous system. When sympathetic activation (“fight or flight”) is elevated, pain sensitivity can increase.
Some PEMF devices use low-frequency waveforms designed to align with relaxation-associated neural rhythms. Users often describe subtle calming sensations during sessions — which may indirectly influence how discomfort is perceived.
This does not mean PEMF treats anxiety or eliminates pain signals. Rather, it may contribute to an environment where the nervous system is less reactive.
In everyday terms, a less reactive nervous system can mean reduced “guarding,” less muscle tension around sensitive areas, and improved tolerance for gentle movement. These are indirect pathways — but they can matter, because tension and vigilance often amplify discomfort.
Some users track changes in relaxation using subjective cues like easier breathing, a calmer baseline, or smoother sleep onset after evening sessions. These are not clinical outcomes, but they are consistent with the idea that autonomic state influences pain perception.
A cautious framework is to treat PEMF as one possible input that supports downshifting — similar to how slow breathing, warmth, or a quiet environment can support nervous system settling. The goal is not to “treat” anything, but to support a context in which discomfort is less amplified.
What Research Actually Shows

Clinical research on PEMF therapy for pain relief is mixed and context-dependent. Studies vary widely in:
- Frequency and waveform
- Intensity levels
- Duration of sessions
- Condition studied
Some trials suggest modest improvements in certain musculoskeletal discomfort patterns. Others show minimal difference compared to placebo.
The key takeaway: PEMF therapy appears most promising as a supportive modality — not a standalone solution. Expectations should remain moderate.
When interpreting PEMF research, it helps to keep a few realities in mind:
- Dose matters: “PEMF” is not one standardized protocol, and outcomes can depend on frequency, intensity, and exposure time.
- Population matters: Results in a narrow study group may not generalize to other contexts.
- Placebo response is real: Pain outcomes are influenced by expectation, attention, and supportive routines.
- Endpoints differ: Some studies measure pain scores, while others measure function, stiffness, or quality-of-life proxies.
This is why PEMF therapy for pain relief is best evaluated using a “weight of evidence” mindset rather than looking for a single definitive study. If a device category is supported by multiple modest findings and aligns with plausible physiology, it may be reasonable to consider — while still keeping expectations conservative.
For readers who want a structured comparison of home systems and mats, our Best PEMF Devices & Mats (2026 Buyer’s Guide) summarizes categories, typical configurations, and what to look for in published specs.
Practical Use Patterns

Typical home users integrate PEMF sessions into a routine:
- 15–30 minutes per session
- Once or twice daily
- Targeted placement for localized areas
- Full-body mat sessions for systemic support
Consistency appears more important than intensity. For a broader overview of system types and configurations, see our Best PEMF Devices & Mats (2026 Buyer’s Guide).
Limits & Contraindications

PEMF therapy for pain relief has limits. It does not:
- Repair structural damage instantly
- Replace physical therapy or rehabilitation
- Diagnose underlying causes of pain
- Serve as a cure for chronic medical conditions
Individuals with implanted electronic devices, active medical conditions, or pregnancy should consult a healthcare professional. See our PEMF Therapy Benefits (Science-Backed Overview) for broader context and our Blog for related topics.
From an ownership and compliance standpoint, it’s also important to treat PEMF devices as wellness tools that require thoughtful use:
- Know your contraindications: Implanted electronic devices (such as pacemakers) and certain medical circumstances may make PEMF inappropriate without clinician guidance.
- Start conservatively: If you are new to PEMF, lower settings and shorter sessions are a reasonable approach while observing how you respond.
- Watch for “too much, too soon” signals: Some people report transient sensations such as unusual alertness, restlessness, or temporary discomfort changes when they increase exposure quickly. If that happens, reducing session time or intensity is a cautious response.
Maintenance and long-term use are often overlooked. Full-body mats and systems can be a meaningful investment, so consider practical realities like:
- Space and setup: Where will you store the mat or coil, and how quickly can you set it up for consistent use?
- Cleaning and care: Follow manufacturer guidance for wiping surfaces and avoiding moisture intrusion into electronic components.
- Routine sustainability: A modest protocol done consistently is often more realistic than an aggressive schedule that is difficult to maintain.
- Tracking expectations: For pain-related goals, it can be more useful to monitor function (ease of movement, recovery time, stiffness patterns) than chasing day-to-day pain score fluctuations.
If pain is new, severe, or progressively worsening, the safest path is medical evaluation to rule out conditions that require professional care. PEMF should sit after that baseline safety step, not before it.
Acute vs Chronic Pain Context

Acute discomfort — such as post-exercise soreness — differs biologically from chronic pain patterns. Acute pain is often inflammatory and short-lived. Chronic pain may involve central sensitization, where the nervous system amplifies signals.
PEMF may be more plausibly aligned with recovery-related discomfort than complex, long-standing centralized pain conditions. This distinction helps set realistic expectations.
Combining PEMF With Broader Recovery Strategies

Most users who explore PEMF therapy for pain relief combine it with:
- Mobility work
- Hydration
- Sleep optimization
- Strength training or rehabilitation exercises
As part of a comprehensive recovery framework, PEMF may contribute to overall tissue support and comfort.
Is PEMF Therapy Right for Your Situation?

If your discomfort is mild to moderate and related to physical activity or daily strain, PEMF may be worth exploring as a low-risk supportive modality.
If pain is severe, worsening, or unexplained, medical evaluation should come first. PEMF is a tool — not a diagnosis.
For a device comparison overview, start with our Buyer’s Guide. If you have questions about our research standards, visit the Contact PEMF Sage page.
Conclusion
PEMF therapy for pain relief operates through plausible physiological pathways involving cellular signaling, circulation, and nervous system regulation. Research suggests modest supportive potential — not dramatic cures.
Used consistently and realistically, PEMF may complement broader recovery strategies. Start with education, review device categories carefully, and maintain expectations aligned with current evidence.
If you want to compare device types and see how home mats and systems differ in features and use cases, begin with the Best PEMF Devices & Mats (2026 Buyer’s Guide).
