PEMF Therapy for Sleep Quality

PEMF therapy for sleep quality is often discussed in the context of nervous system regulation, relaxation support, and circadian balance. As more people explore non-pharmacologic approaches to winding down at night, interest in pulsed electromagnetic field therapy has expanded beyond pain and recovery into the realm of restorative rest.
This guide explains how PEMF may influence sleep physiology, what current research suggests, and where realistic expectations should be placed. The tone here is conservative and evidence-aligned: PEMF is not a sedative, not a treatment for insomnia, and not a substitute for medical care. Instead, it may function as a supportive tool within a broader sleep hygiene strategy.
Understanding Sleep Physiology

Sleep is regulated by two major systems: the circadian rhythm (your internal clock) and the sleep pressure system that builds throughout the day. According to the National Institutes of Health (NIH), consistent sleep timing, light exposure, and nervous system balance are central to maintaining restorative sleep cycles.
When the sympathetic (“fight-or-flight”) system remains elevated at night, falling asleep and staying asleep can become more difficult. This is where interest in PEMF therapy for sleep quality typically begins — not as a direct sleep inducer, but as a potential modulator of autonomic balance.
How PEMF May Influence the Nervous System
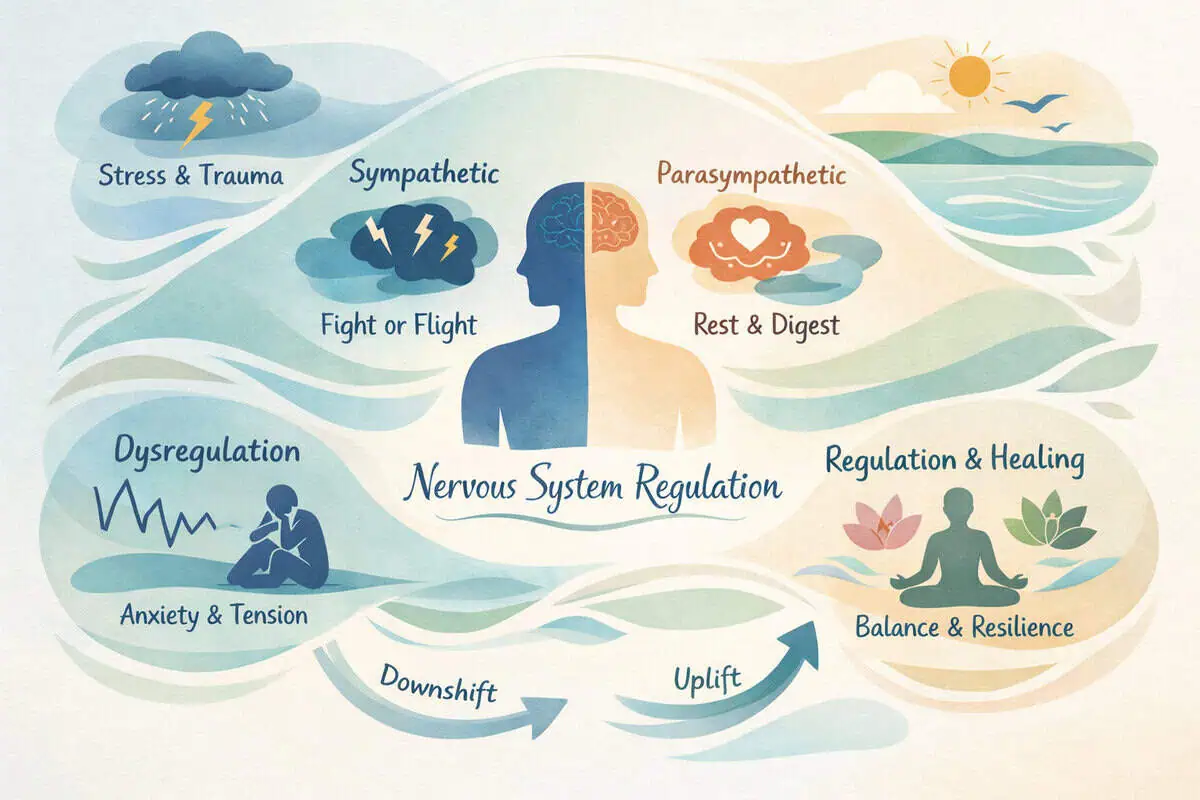
PEMF therapy delivers low-frequency electromagnetic pulses that interact with cellular signaling pathways. Research has explored how these signals may influence ion channel activity and membrane potential, which in turn can affect nerve signaling patterns. Some studies indexed on PubMed suggest low-frequency electromagnetic exposure may influence autonomic tone under controlled conditions.
In practical terms, users often describe sessions as subtly pulsing and relaxing rather than stimulating. While experiences vary, sessions are typically performed lying down for 15–30 minutes, which itself reinforces a wind-down routine.
From a physiology framing standpoint, “autonomic balance” refers to how the sympathetic and parasympathetic systems shift throughout the day. At night, many people aim for parasympathetic dominance — a state associated with slower breathing, lower perceived stress, and less muscle tension. A PEMF session used in the evening is often intended to support that transition, not to “knock someone out” or force sleep.
It is also helpful to separate two ideas that can get blended together online:
- Immediate sensations: some people feel warmth, subtle pulsing, or a mild calming effect during a session.
- Downstream outcomes: improvements in sleep continuity or perceived restfulness are more complex and depend on many variables (routine consistency, timing, sleep environment, and individual sensitivity).
If PEMF is used too close to bedtime at higher intensity (depending on the device), some individuals report feeling “alert” rather than calm. That does not mean PEMF is harmful, but it does reinforce why conservative settings and predictable timing are often preferred when the goal is relaxation support.
Circadian Rhythm & Electromagnetic Signaling
Circadian rhythm is influenced by light exposure, hormonal patterns, and cellular metabolic timing. Melatonin production, core body temperature changes, and mitochondrial signaling all follow rhythmic cycles.
PEMF therapy for sleep quality is theorized to support cellular communication and mitochondrial efficiency. While this does not equate to altering melatonin directly, improved cellular signaling and microcirculatory support may indirectly reinforce nighttime recovery patterns.
For a broader overview of how PEMF affects biological systems, see our science-backed overview of PEMF therapy benefits.
A circadian-friendly evening routine typically reduces “wake signals” (bright light, heavy meals, intense work, stressful conversations) and increases “sleep signals” (dim lighting, consistent timing, calm activities). Within that frame, PEMF is often positioned as one part of a broader wind-down pattern rather than a standalone intervention.
Microcirculation & Relaxation Support

Healthy sleep involves coordinated blood flow shifts and parasympathetic dominance. Research has examined how electromagnetic stimulation may influence microcirculation and endothelial function. The Cleveland Clinic notes that circulation plays a role in tissue oxygenation and recovery processes that occur overnight.
By potentially supporting microcirculatory patterns, PEMF sessions may complement relaxation routines. Importantly, these effects are supportive rather than curative and should be viewed within the larger context of sleep hygiene.
Microcirculation is often discussed because it reflects the “last mile” of blood flow — the small vessels involved in oxygen and nutrient delivery. For some individuals, bedtime discomfort, muscle tightness, or general restlessness can make it harder to settle. A calming session that supports relaxation (and possibly local comfort) may indirectly improve the ability to wind down.
It is also worth stating what this does not mean. Improved circulation support does not automatically translate into predictable changes in sleep architecture, and it does not override other common disruptors like caffeine timing, alcohol, screen exposure, or an inconsistent sleep schedule.
A conservative and practical approach is to treat microcirculation support as one possible “supportive layer” in a stack that also includes:
- a cooler sleep environment,
- reduced late-night stimulation,
- a consistent pre-bed routine, and
- appropriate evaluation if symptoms suggest a sleep disorder.
Mitochondrial Function & Overnight Recovery

Mitochondria are responsible for ATP production and cellular energy regulation. Some experimental research has explored how pulsed electromagnetic fields may influence mitochondrial membrane potential and ATP output.
Sleep itself is a metabolic reset period. While PEMF therapy for sleep quality is not a replacement for sleep, some individuals use evening sessions as part of a recovery-oriented routine designed to align with the body’s natural energy recalibration.
From a conservative perspective, it helps to keep “mitochondrial support” language grounded. Mitochondria are involved in energy production, signaling, and oxidative balance, and the body’s overnight recovery processes are coordinated across many systems (metabolic, immune signaling, nervous system regulation). PEMF research in this area is not uniform, and results often depend on dosing factors such as intensity, waveform, and duration.
A practical takeaway for readers is not that PEMF “boosts ATP” in a guaranteed way, but that some users choose it as a low-effort recovery adjunct. If the session reduces perceived tension and supports a calmer pre-sleep state, that alone can make sleep routines easier to maintain — which is often the main driver of change over time.
If you want a deeper, PEMF-specific overview of how mechanisms are discussed across the literature (with conservative framing), the related concepts are also covered across our educational content in the PEMF Sage blog.
What Research Currently Suggests

Clinical literature evaluating PEMF and sleep specifically remains limited. Some small-scale studies have examined electromagnetic field exposure and subjective sleep quality, though results vary depending on frequency, intensity, and population studied.
The Mayo Clinic emphasizes that foundational sleep practices — consistent timing, reduced evening light exposure, stress reduction, and limiting stimulants — remain primary drivers of sleep improvement.
PEMF may serve as an adjunctive tool rather than a primary intervention.
When reviewing claims about PEMF therapy for sleep quality, a helpful evidence-aligned checklist is to ask:
- What outcome was measured? (subjective sleep quality, sleep latency, awakenings, or objective sleep staging)
- What dosing was used? (frequency range, intensity, session duration, and program type)
- Who was studied? (healthy adults, athletes, older adults, or people with specific symptoms)
- Was there a control group? (to reduce expectation effects)
Because sleep is sensitive to expectation, environment, and routine, it is possible for supportive interventions to “work” in the sense that they help someone feel calmer and more consistent with bedtime — even when direct physiological effects on sleep architecture are uncertain. That does not invalidate a supportive routine, but it does mean results should be interpreted carefully and without guarantees.
For readers who want to explore the broader research landscape and how PEMF studies are typically structured, our cornerstone comparisons in the 2026 Buyer’s Guide can help contextualize device categories and claims in a conservative way.
Typical Evening Usage Patterns

Users who incorporate PEMF therapy for sleep quality often:
- Schedule sessions 30–60 minutes before bedtime
- Use lower-intensity relaxation programs
- Combine sessions with breathing exercises
- Dim lights during treatment
Consistency appears more important than intensity. A calm, predictable evening environment likely contributes as much to results as the device itself.
A conservative “routine builder” approach is to treat PEMF as a cue that the day is winding down. Many people pair a session with low-stimulation habits such as:
- reading (paper or e-ink rather than bright screens),
- gentle stretching or mobility work,
- slow nasal breathing, or
- light journaling to offload next-day tasks.
If you are testing PEMF therapy for sleep quality, it can be useful to track a simple baseline for 1–2 weeks before changing too many variables. For example: bedtime consistency, estimated time to fall asleep, number of awakenings, and morning freshness. This makes it easier to notice whether any changes appear tied to consistency rather than a one-off session.
One additional practical point: many users prefer to complete a session before getting into bed, especially if the device setup requires adjusting cables or controls. Keeping the bed primarily associated with sleep (and not fiddling with equipment) can support better conditioning over time.
Safety & Contraindications

PEMF therapy is generally considered low-risk when used appropriately. However, individuals with implanted electronic devices, pacemakers, pregnancy, or seizure disorders should consult a healthcare professional before use.
For a detailed breakdown of safety considerations, review our PEMF therapy safety and contraindications guide.
In addition to medical contraindications, there are practical safety considerations that matter for home ownership:
- Follow manufacturer guidance: device-specific rules for distance, placement, and intensity are not interchangeable between brands.
- Avoid “overnight use” assumptions: most users treat PEMF as a session-based tool rather than something left running unattended during sleep.
- Be cautious with combined modalities: stacking heat, stimulants, or intense exercise late at night can complicate sleep outcomes and make cause-and-effect unclear.
If you have complex medical history, implanted devices, or are under active care for a sleep disorder, the safest approach is to discuss PEMF with your clinician and bring device specifications if possible. If you have general questions about how we approach safety and evidence standards, you can also reach us via the Contact PEMF Sage page.
Finally, long-term use is usually about maintenance and routine consistency rather than “pushing intensity.” Clean setup, stable placement, and predictable timing are often more relevant to a sleep-focused routine than aggressive settings.
Comparing PEMF to Other Sleep Supports

Unlike melatonin supplements or prescription sleep aids, PEMF therapy for sleep quality does not act as a chemical sedative. Its proposed mechanism centers on physiological signaling rather than hormone replacement.
This makes it fundamentally different from pharmacologic approaches — but also means expectations should be aligned accordingly.
In the broader sleep landscape, many evidence-aligned tools target different levers:
- Behavioral approaches: consistent schedule, stimulus control, and structured routines (often the highest leverage).
- Environment changes: darkness, reduced noise, cooler temperature, and limiting screens.
- Relaxation practices: breathing exercises, progressive muscle relaxation, mindfulness, or gentle stretching.
PEMF tends to fit most naturally into the “relaxation practice” category: a structured, time-boxed session that encourages stillness and downshifting. For some people, that structure is the primary benefit. For others, PEMF may be neutral — and that is an acceptable outcome when expectations remain conservative.
When to Consider Broader Evaluation

Persistent insomnia, loud snoring, breathing interruptions, or severe daytime fatigue warrant medical evaluation. Sleep apnea and other disorders require professional diagnosis and management.
PEMF therapy may complement, but never replace, appropriate medical care.
A conservative “red flag” list for seeking evaluation sooner rather than later includes:
- waking up gasping or choking,
- unrefreshing sleep despite adequate time in bed,
- significant daytime sleepiness that affects driving or work,
- unexplained morning headaches, or
- restless legs symptoms that repeatedly disrupt sleep.
In these cases, it is more productive to identify the underlying issue than to keep adding new wellness tools. PEMF can still be used cautiously as part of a comfort-focused routine, but it should not delay evidence-based evaluation and treatment when indicated.
Choosing a Device for Home Use

If exploring home devices, look for:
- Low-frequency options suitable for relaxation programs
- Adjustable intensity settings
- Clear manufacturer specifications
Our 2026 Buyer’s Guide to the best PEMF devices outlines differences between mat systems and professional-grade platforms in a conservative, comparison-based format.
For sleep-focused use, selection often comes down to practical factors more than marketing language. Examples include:
- Ease of setup: a device that is simple to place and start is more likely to be used consistently.
- Program design: availability of lower-intensity or relaxation-oriented modes that feel comfortable in the evening.
- Adjustability: the ability to dial intensity down rather than being locked into one strong setting.
- Noise and controls: quiet operation and dimmable or unobtrusive displays can matter if the goal is winding down.
Device category can also influence how people use PEMF therapy for sleep quality:
- Full-body mats: often used lying down, which naturally pairs with pre-bed routines and relaxation practices.
- Targeted applicators: sometimes used for localized comfort earlier in the evening, then followed by standard sleep hygiene steps.
- Clinic-style systems: typically session-based and less integrated into nightly routines due to access and scheduling.
Regardless of category, a conservative approach is to start with short sessions, lower intensity, and stable timing for at least 1–2 weeks. If the routine is not helping (or feels stimulating), it may be better to adjust timing, reduce intensity, or discontinue rather than forcing it.
Conclusion
PEMF therapy for sleep quality is best understood as a supportive wellness tool rather than a direct sleep treatment. Its potential influence on nervous system balance, microcirculation, and cellular signaling may complement consistent sleep routines.
For readers exploring structured device comparisons, visit our comprehensive PEMF Buyer’s Guide or browse the full PEMF Sage blog for additional evidence-aligned resources.
If sleep symptoms are persistent, severe, or disruptive, consider medical evaluation so that supportive tools like PEMF are used appropriately within a broader plan.
