PEMF Therapy and Circulation

PEMF therapy and circulation are often discussed together because cellular signaling, vascular tone, and microcirculatory dynamics all play central roles in how tissues receive oxygen and nutrients. Pulsed electromagnetic field therapy does not “push” blood through vessels directly. Instead, it is studied for how it may influence cellular communication, ion exchange, and endothelial responsiveness — all of which contribute to healthy circulatory function.
This guide explains what circulation actually means, how microcirculation differs from general blood flow, and how PEMF therapy is evaluated in the context of vascular signaling — using conservative, physiology-aligned language.
What “Circulation” Actually Refers To

Circulation refers to the movement of blood through arteries, capillaries, and veins. It supports:
- Oxygen delivery
- Nutrient transport
- Metabolic waste removal
- Thermal regulation
Large-vessel blood flow (macrocirculation) is controlled primarily by cardiac output and vascular resistance. In contrast, microcirculation — the flow through tiny capillaries — depends heavily on local signaling at the cellular and endothelial level.
To better understand these mechanisms, see our foundational guide on PEMF therapy benefits, which explains how signaling processes relate to broader physiological function.
It also helps to separate a few closely related terms that are often blurred together in everyday conversation:
- Perfusion is the delivery of blood to a tissue bed (often discussed at the capillary level).
- Vascular tone is the “set point” of constriction vs. dilation in vessels, shaped by nervous system input and local signals.
- Capillary exchange is the movement of oxygen, nutrients, and fluid across capillary walls into tissues.
- Venous return is the flow of blood back to the heart, influenced by valves, muscle contraction, and pressure gradients.
When someone says they want to “boost circulation,” they may be referring to warmth, recovery, comfort, or a subjective sense of flow. Those experiences can be real, but they are not the same thing as measured changes in perfusion, vessel diameter, or microvascular exchange.
Finally, circulation is influenced by everyday variables that can confound interpretation. Hydration status, ambient temperature, stress load, caffeine or nicotine exposure, recent exercise, and sleep quality can all shift vascular tone and peripheral blood flow. That context matters when evaluating any wellness tool discussed alongside circulation.
The Endothelium: A Signaling Interface
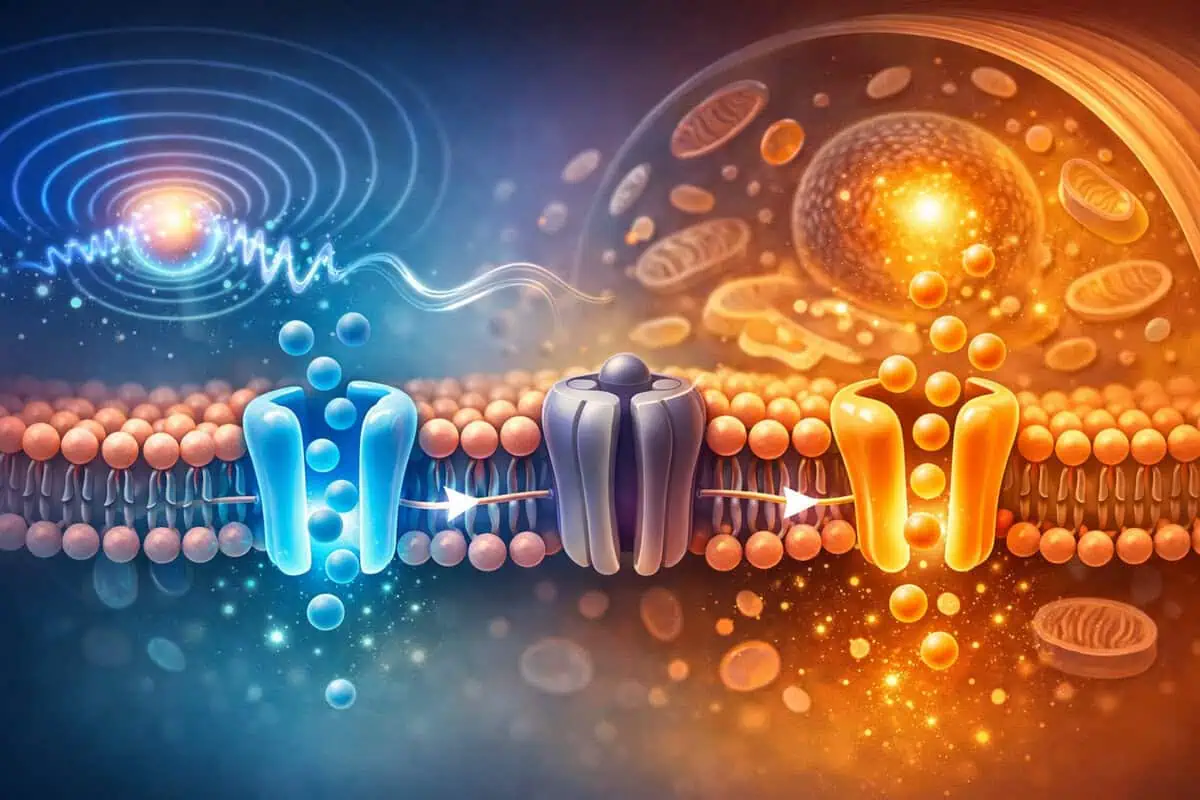
The inner lining of blood vessels — known as the endothelium — is not simply structural. It acts as an active signaling surface that regulates vascular tone, nitric oxide production, and capillary responsiveness.
Research published in PubMed-indexed studies has explored how electromagnetic field exposure may influence ion channel behavior and nitric oxide signaling pathways. These processes are relevant because nitric oxide contributes to vasodilation — the natural widening of blood vessels.
PEMF therapy is studied in this context as a modulator of cellular electrical gradients rather than a mechanical pump.
A practical way to think about endothelial function is that it helps vessels “listen” and “respond” to changing needs. When a tissue becomes more active (during movement, temperature changes, or local metabolic demand), chemical messengers and mechanical forces can signal the endothelium to adjust vessel diameter and capillary recruitment.
One of the most discussed endothelial pathways is nitric oxide signaling, which can be triggered by a combination of biochemical cues and shear stress (the frictional force of blood moving along vessel walls). That is one reason why exercise can support endothelial responsiveness: it naturally increases shear stress and stimulates adaptive signaling.
Within conservative PEMF discussions, the question is not whether PEMF replaces these foundational mechanisms. The more restrained framing is whether certain PEMF parameters may influence cellular signaling environments in a way that is directionally consistent with healthy vascular responsiveness in some settings, while recognizing that outcomes vary and may not translate uniformly across populations.
Importantly, endothelial function is not a single switch. It reflects a dynamic balance between vasodilatory and vasoconstrictive signals, oxidative stress buffering, inflammation signaling, and autonomic input. Any claim that a modality “optimizes” the endothelium in all cases would be overstated.
Microcirculation vs. General Blood Flow

When people refer to “improving circulation,” they often mean improving comfort, warmth, or recovery. However, physiologically speaking, microcirculation involves:
- Capillary density
- Red blood cell flexibility
- Local oxygen diffusion gradients
- Endothelial responsiveness
Studies discussed by the National Institutes of Health (NIH) highlight how microvascular function is tightly regulated by cellular communication rather than gross mechanical force.
PEMF therapy and circulation research often centers on these micro-level mechanisms.
Microcirculation is where “delivery” becomes “exchange.” Even if large vessels are functioning normally, tissues still depend on:
- Capillary recruitment (how many capillaries are actively perfused at a given time)
- Transit time (how long red blood cells remain in capillary beds, affecting exchange opportunity)
- Diffusion distance (how far oxygen must travel from capillary to cell)
- Blood rheology (flow properties such as viscosity and the deformability of red blood cells)
That is one reason why microcirculation is often discussed in recovery contexts: the capillary environment is where oxygen delivery, waste removal, and nutrient exchange occur at a practical level. However, this does not mean that every subjective sensation of warmth or relaxation reflects a measurable shift in capillary function.
From an evaluation standpoint, studies that discuss microcirculation may use tools such as laser Doppler flowmetry, tissue oxygenation measures, or microvascular reactivity tests. These endpoints are specific and context-dependent. They also highlight why broad claims can be difficult to validate without standardized protocols and adequate study size.
In conservative terms, PEMF-related discussions about microcirculation are best interpreted as hypothesis-driven and mechanism-oriented, rather than as guarantees of consistent, real-world perfusion changes for every user.
Cellular Signaling and Ion Exchange
Cells maintain electrical gradients across membranes. These gradients influence:
- Calcium influx
- Sodium-potassium balance
- ATP production efficiency
Because vascular smooth muscle contraction depends on calcium signaling, any modulation of ion channel dynamics may indirectly affect vessel tone.
Our overview of Best PEMF Devices & Mats (2026 Buyer’s Guide) explains how field intensity and waveform variability are designed to remain within conservative wellness parameters.
PEMF parameters matter because different settings can produce different induced electrical effects in tissues. In general discussions, people may refer to:
- Frequency (Hz) — how often the pulse repeats
- Waveform — the shape of the pulse (which affects rise time and exposure pattern)
- Intensity — often reported in gauss or tesla units at the coil (not necessarily the same as tissue-level exposure)
- Duty cycle — how long the signal is “on” vs. “off” over a given period
Mechanistically, the restrained framing is that time-varying electromagnetic fields can induce small electric fields that may interact with charged particles and membrane processes. This is often discussed in relation to ion channels and membrane potential stability. It is not typically framed as a direct “blood flow” intervention, but as a signaling-oriented modality that could influence upstream regulators of vascular behavior in some contexts.
Because the relationship between device specs and tissue-level effects is complex, it is wise to treat spec comparisons as one input rather than a definitive predictor of outcomes. Coil geometry, distance from the body, user positioning, and session consistency can all change exposure conditions in real-world use.
Circulation and Oxygen Delivery

Oxygen delivery depends on hemoglobin binding capacity and capillary exchange efficiency. The Cleveland Clinic explains that tissue oxygenation is influenced not only by heart output but by microvascular integrity.
PEMF therapy and circulation discussions frequently reference how improved endothelial responsiveness may support oxygen diffusion at the tissue level — though this remains an area of ongoing investigation.
At a basic physiology level, oxygen delivery depends on multiple steps working together:
- Oxygen entering the lungs and binding to hemoglobin
- Blood being circulated to tissues (macro-level flow)
- Capillary exchange and diffusion into cells (micro-level delivery)
- Cellular utilization of oxygen within mitochondria
This “chain” framing matters because a change in one link does not automatically improve the whole system. For example, a person can have adequate macro-level circulation but still experience local delivery constraints related to microvascular reactivity, tissue swelling, diffusion distance, or autonomic constriction in peripheral beds (especially under stress or cold exposure).
As a result, any wellness discussion about supporting oxygen delivery should stay conservative and multi-factor. PEMF-related hypotheses about oxygenation are usually discussed through microcirculatory signaling and endothelial pathways rather than as a substitute for foundational behaviors like movement, sleep, hydration, and clinician-guided care when indicated.
Nervous System Regulation and Vascular Tone
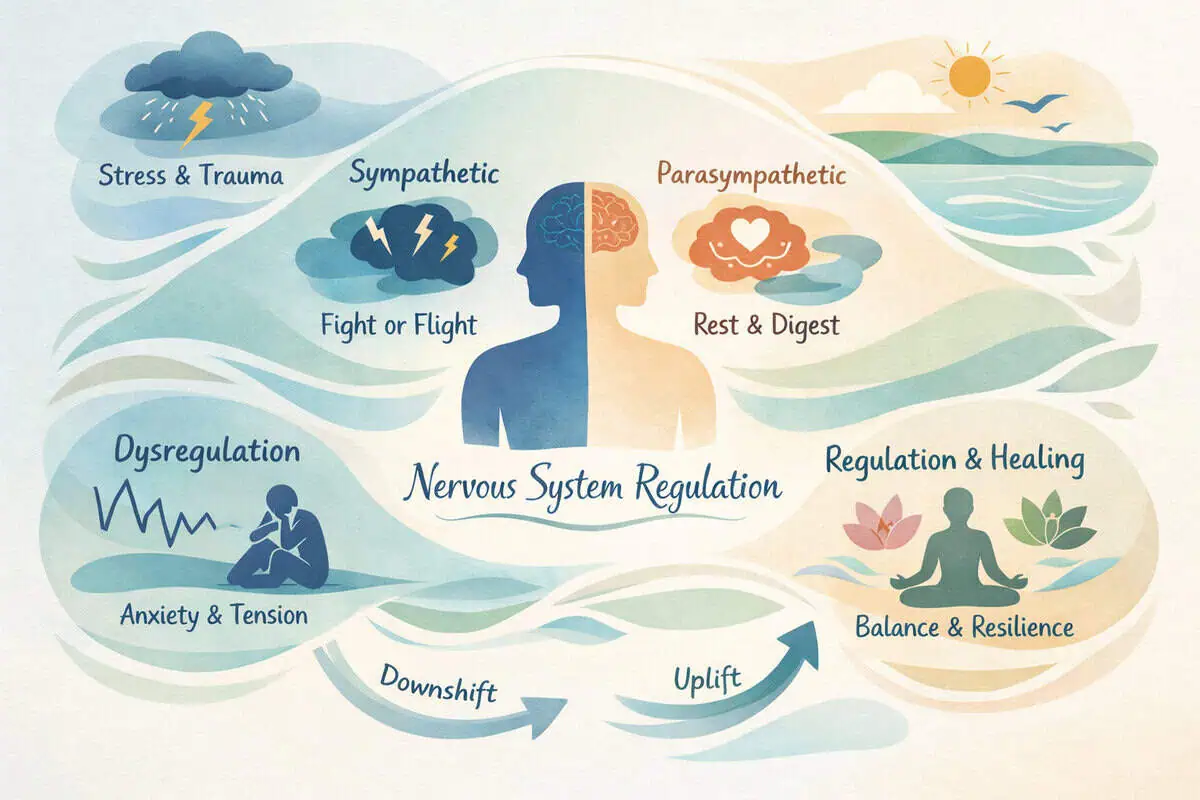
The autonomic nervous system plays a major role in vascular tone. Sympathetic activation can constrict vessels, while parasympathetic dominance supports relaxation responses.
PEMF therapy has been studied for how it may interact with autonomic balance, which could indirectly influence circulation patterns. For a broader overview of how these mechanisms intersect, explore additional educational articles in our Blog.
In practical terms, many circulation-related sensations are strongly influenced by autonomic state. Under sympathetic load (stress, time pressure, high arousal), peripheral vessels can constrict, and hands or feet may feel colder. During relaxation, peripheral vasodilation may increase, which can change perceived warmth and comfort.
That does not mean every relaxation response equals “improved circulation” in a clinical sense. It does suggest that routines that downshift autonomic tone — breathwork, consistent sleep habits, and gentle recovery practices — can influence vascular tone and subjective comfort through well-established pathways.
Within conservative PEMF framing, the question becomes whether PEMF sessions that users associate with relaxation may align with a broader parasympathetic-supportive routine. Any downstream vascular effects, if present, would be interpreted as indirect and context-dependent rather than automatic or universal.
How PEMF Is Typically Used in Wellness Routines

Observed usage patterns often include:
- 20–30 minute sessions
- Full-body mat placement
- Evening or recovery-focused routines
- Low-to-moderate intensity settings
Users frequently describe subtle pulsing sensations or a general sense of warmth and relaxation. These experiential observations are separate from measurable hemodynamic outcomes.
What Current Research Suggests — and Its Limits

The Mayo Clinic and other institutions emphasize that electromagnetic therapies should be viewed within evidence-based boundaries. While laboratory and small-scale studies have explored vascular effects, large-scale clinical consensus is still evolving.
PEMF therapy should not be viewed as a replacement for cardiovascular medical care, prescription therapies, or physician-guided treatment plans.
A measured way to interpret the research is to look at three layers of evidence:
- Mechanistic plausibility (cell signaling pathways that could relate to vascular tone or microvascular responsiveness)
- Physiological endpoints (microcirculation measurements, tissue oxygenation signals, or vascular reactivity tests)
- Meaningful real-world outcomes (functional comfort, routine adherence, or clinician-supervised metrics when applicable)
Many PEMF discussions around circulation sit primarily in the first two layers. That is not inherently negative, but it does mean users should avoid jumping from a plausible mechanism to a guaranteed outcome. Differences in device settings, study protocols, participant characteristics, and measurement tools can all change what results mean.
It is also important to recognize that circulation-related research can be sensitive to confounders. Temperature, posture, stress, recent exercise, hydration, and sleep can shift vascular tone. Without careful controls, it can be difficult to attribute changes to a single input.
For readers who want a practical “ownership reality” lens: a PEMF device should be viewed as a routine-based tool. Benefits — if experienced — often align with consistency, conservative settings, and integration into broader lifestyle supports. In contrast, irregular or high-variability use can make it hard to know what is driving changes in comfort or perceived circulation.
From a long-term perspective, it can also be helpful to set modest evaluation checkpoints. Some users track session consistency, sleep timing, perceived warmth or comfort, and recovery readiness alongside stable variables like daily movement and hydration. This does not prove causality, but it supports clearer self-observation and safer expectations.
Safety and Circulatory Considerations

Individuals with implanted electronic devices, certain cardiovascular conditions, or pregnancy should consult a qualified healthcare professional before use.
For detailed contraindications and risk factors, review our PEMF therapy safety page.
For circulation-related conversations specifically, “more intensity” is not a safety strategy. Conservative use typically prioritizes comfort, adherence, and alignment with manufacturer guidance, especially for users who are medically complex or who are coordinating care with a clinician.
Avoiding Overstated Performance Claims

It is important to distinguish between:
- Supporting physiological signaling
- Claiming medical treatment outcomes
PEMF therapy and circulation discussions should remain grounded in cellular communication research — not disease-specific or cure-oriented claims.
Who Might Explore PEMF for Circulatory Support

Individuals interested in general wellness, recovery routines, or microcirculatory research may explore this topic further. PEMF therapy is typically positioned within a broader lifestyle framework that includes:
- Physical activity
- Balanced nutrition
- Sleep hygiene
- Medical oversight when necessary
It may be especially relevant for readers who want a conservative, non-pharmacologic routine tool and who are comfortable evaluating outcomes in terms of comfort, routine consistency, and general wellness support rather than disease-specific targets.
PEMF Therapy and Circulation: A Measured Perspective
PEMF therapy and circulation intersect at the level of cellular signaling, endothelial responsiveness, and nervous system balance. Rather than mechanically forcing blood flow, pulsed electromagnetic fields are studied for how they may influence the communication systems that help regulate vascular tone and microcirculation.
If you’re exploring device options or want to understand how different systems are designed, review our comprehensive Buyer’s Guide to PEMF devices for a conservative comparison framework.
